Your stomach has always known things before your brain caught up. That nervous feeling before a big moment, the sudden appetite loss during stress, or that heavy gut feeling when something is just not right. These are not coincidences. They are your body’s most fascinating internal conversation, and science has finally started to understand it deeply. The Gut-Brain Connection is one of the most exciting and rapidly growing areas of health research today, and understanding it could genuinely change the way you approach your mental and physical wellbeing.
What Exactly Is The Gut-Brain Connection?
- The Gut-Brain Connection, scientifically referred to as the gut-brain axis, is the bidirectional communication network between your gastrointestinal tract and your central nervous system. In simple terms, your gut and your brain are constantly talking to each other through nerves, hormones, and chemical signals. This is not a one-way street where only the brain gives orders to the gut. The gut sends just as many signals back up to the brain, influencing your mood, thoughts, emotions, and even decision-making.
- The gut-brain axis is the network of nerves that connect your brain and gut and send signals back and forth, and your nervous system also works closely with your endocrine system, which produces hormones that communicate things like hunger, fullness, and stress.
- What makes this even more remarkable is the sheer scale of the gut’s nervous system. The enteric nervous system, often called the “second brain,” contains over 500 million neurons lining your gastrointestinal tract. This system operates largely independently, which is why your gut keeps functioning even when your spinal cord is severed. It is a brain within a body, quietly running the show from below.
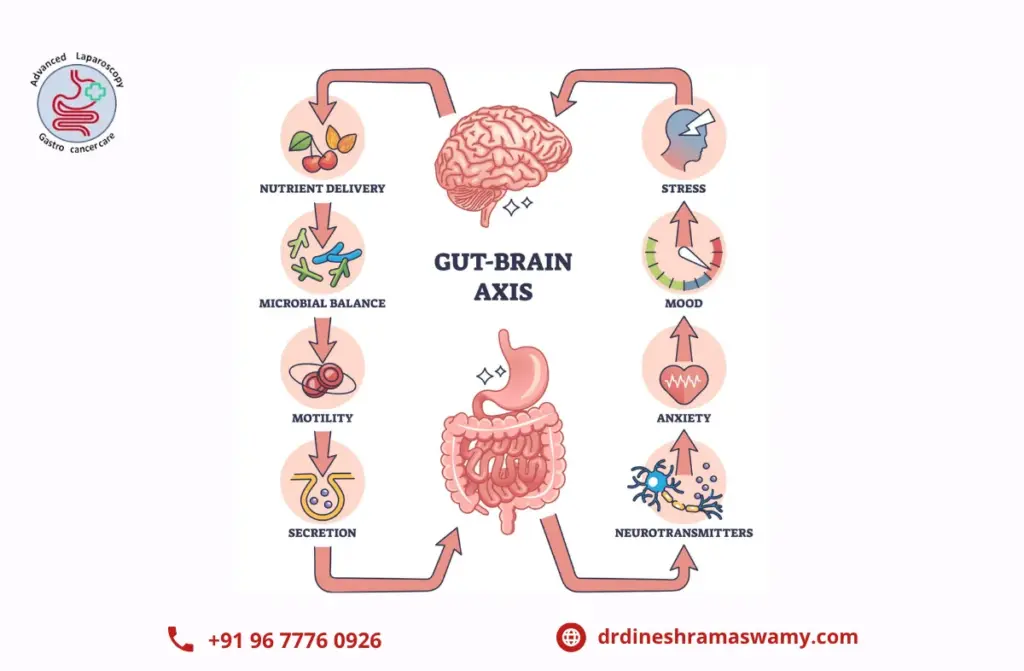
The Vagus Nerve: The Superhighway of Gut-Brain Communication
- At the heart of The Gut-Brain Connection is the vagus nerve, the longest cranial nerve in your body. It runs from the brainstem all the way down to the abdomen, acting as a direct telephone line between your gut and your mind. Through direct signals from the vagus nerve, which connects the brain and the gut, as well as through molecules secreted into the bloodstream from gut microbes and immune cells that traffic from the gut to the rest of the body, the brain and digestive tract are in constant communication.
- When this communication flows smoothly, you feel balanced, calm, and well. But when signals are disrupted, the consequences can range from digestive discomfort to anxiety, depression, and even cognitive difficulties. Researchers are now investigating vagus nerve stimulation as a potential treatment for depression, a finding that would have seemed unimaginable just two decades ago.
Your Gut Microbiome: The Invisible Brain Influencer
- Trillions of bacteria, fungi, and other microorganisms live inside your gut. Collectively called the gut microbiome, these tiny organisms are far more influential than most people realise. They do not just help digest food. They produce neurotransmitters, regulate inflammation, and communicate directly with your brain.
- Notable biological functions of the gut microbiome include secretion of neuroactive substances, including serotonin, dopamine, and gamma-aminobutyric acid (GABA), which influence behaviour, cognition, and emotions.
- Here is a staggering fact: approximately 90 to 95 percent of your body’s serotonin, the neurotransmitter most associated with happiness and mood regulation, is produced in the gut, not the brain. This single discovery has reshaped how researchers think about depression, anxiety, and mental wellbeing. When your gut microbiome is healthy and diverse, serotonin production is stable. When it is disrupted, your mood often follows.
- The Gut-Brain Connection becomes even more significant when you consider that an imbalanced microbiome, known as dysbiosis, has been linked to conditions including irritable bowel syndrome, anxiety disorders, depression, autism spectrum disorder, and even Parkinson’s disease.
Gut Health and Mental Health: A Two-Way Road
- One of the most important things to understand about the gut-brain connection is that influence flows both ways. Chronic stress weakens the gut lining, disrupts the microbiome, and worsens digestive conditions. At the same time, a damaged gut microbiome sends distress signals to the brain, contributing to low mood and heightened anxiety.
- An imbalance in gut bacteria, known as dysbiosis, causes the barrier between the gut and the bloodstream to become permeable, which can allow bad bacteria to enter the bloodstream, potentially causing inflammation, and dysbiosis also alters the blood-brain barrier, contributing to inflammation of the brain matter.
- This inflammatory cycle explains why people with chronic gut conditions like Crohn’s disease or irritable bowel syndrome often report higher rates of anxiety and depression. It is not simply that being unwell makes you feel sad. The gut inflammation is literally signalling the brain to increase stress responses and reduce mood-regulating chemicals.
- Understanding this cycle is empowering because it means that improving your gut health is one of the most direct and natural ways to support your mental health.
What Damages The Gut-Brain Connection?
Several modern lifestyle habits are quietly disrupting the gut-brain axis every day. Being aware of these is the first step toward protecting this vital communication system.
- Poor diet: Highly processed foods, excess sugar, and low fibre intake starve beneficial gut bacteria and feed harmful ones, disrupting the microbiome rapidly.
- Chronic stress: Prolonged psychological stress reduces gut motility, increases intestinal permeability, and alters the composition of gut bacteria within days.
- Antibiotic overuse: While antibiotics are sometimes necessary, overuse wipes out large populations of beneficial gut bacteria, and recovery can take months or even years without active support.
- Poor sleep: Sleep and gut health are deeply intertwined. Disrupted sleep patterns alter the microbiome, and an unhealthy microbiome disrupts sleep quality, creating a damaging cycle.
- Sedentary lifestyle: Physical inactivity reduces microbial diversity in the gut, which directly weakens the signals travelling through the gut-brain axis.
How to Strengthen The Gut-Brain Connection Naturally
The encouraging reality is that the gut microbiome is highly responsive to lifestyle changes. Small, consistent actions create significant improvements in gut health, which translate directly into better mood, sharper thinking, and lower anxiety levels.
- Eat a diverse, fibre-rich diet: Vegetables, legumes, whole grains, and fruits feed the beneficial bacteria that produce mood-supporting neurotransmitters. Aim for at least 30 different plant foods per week for maximum microbiome diversity.
- Include fermented foods: Yoghurt, kefir, kimchi, sauerkraut, and kombucha introduce beneficial live bacteria directly into the gut. Regular consumption of these foods has been shown in clinical studies to reduce markers of inflammation and improve mood.
- Manage stress actively: Practices like meditation, breathwork, yoga, and spending time in nature activate the vagus nerve and reduce the stress hormones that damage gut lining. Even 10 minutes of daily mindful breathing produces measurable changes in gut-brain signalling.
- Prioritise sleep quality: Seven to nine hours of consistent, quality sleep gives the gut microbiome the recovery time it needs. Avoiding screens before bed and maintaining a regular sleep schedule directly supports gut health.
- Stay physically active: Regular moderate exercise, such as walking, swimming, or cycling, significantly increases microbial diversity and enhances vagal tone, strengthening the gut-brain connection over time.
- Consider probiotics and prebiotics: Probiotic supplements introduce beneficial bacterial strains, while prebiotic foods like garlic, onions, bananas, and oats feed and sustain them. According to research published in the National Institutes of Health, probiotics and prebiotics beneficially modulate microbial and immune pathways to improve brain function.
The Gut-Brain Connection and Common Health Conditions
Research into the gut-brain connection is revealing new links between gut health and conditions that were previously considered purely neurological or psychological.
- Anxiety and depression: Multiple studies now show that patients with anxiety and depression have measurably different gut microbiome compositions compared to healthy individuals. Probiotic interventions have shown promising results in reducing anxiety scores in clinical trials.
- Irritable Bowel Syndrome (IBS): IBS is now understood as a gut-brain disorder rather than a purely digestive one. Psychological therapies like cognitive behavioural therapy have been shown to reduce IBS symptoms, confirming the powerful bidirectional nature of gut-brain communication.
- Alzheimer’s and Parkinson’s disease: Emerging research suggests that neurodegeneration may begin in the gut before it reaches the brain, potentially through the vagus nerve. This opens entirely new possibilities for early detection and prevention through gut health monitoring.
- Autism spectrum disorder: Studies have consistently found altered gut microbiome compositions in individuals with autism, and researchers are investigating whether gut-targeted interventions could support neurological development and reduce certain symptoms.
Conclusion
The Gut-Brain Connection is not a wellness trend or a passing theory. It is a well-established, deeply researched area of science that is actively reshaping how medicine understands mental health, neurological disease, and overall wellbeing. Your gut is listening to your brain, and your brain is listening right back. Taking care of your gut through better food choices, stress management, quality sleep, and physical activity is one of the most powerful investments you can make in your mental and physical health. Start small, stay consistent, and let your gut do what it does best: keep your whole self in balance.