Digestive problems are often ignored as acidity, stress, or irregular eating habits. However, persistent stomach pain, diarrhea, bloating, and unexplained weight loss may be signs of Inflammatory Bowel Disease (IBD), a chronic condition affecting the digestive tract. Commonly seen in young adults and teenagers, IBD can impact daily life, nutrition, and emotional well-being. Early diagnosis and proper treatment can help manage symptoms and improve quality of life.
What Is Inflammatory Bowel Disease (IBD)?
Inflammatory Bowel Disease (IBD) is a chronic condition that causes ongoing inflammation in the digestive tract. Unlike temporary stomach infections, IBD symptoms can flare up repeatedly over time and affect daily life. The condition occurs when the immune system mistakenly attacks the digestive system, leading to pain, ulcers, diarrhea, and digestive discomfort. Many people ignore the early symptoms, assuming they are caused by stress or food habits, which can delay proper diagnosis and treatment.
Types of Inflammatory Bowel Disease
IBD is primarily classified into two major types: Crohn’s Disease and Ulcerative Colitis. While both involve inflammation in the digestive tract, they affect the body differently.
Crohn’s Disease
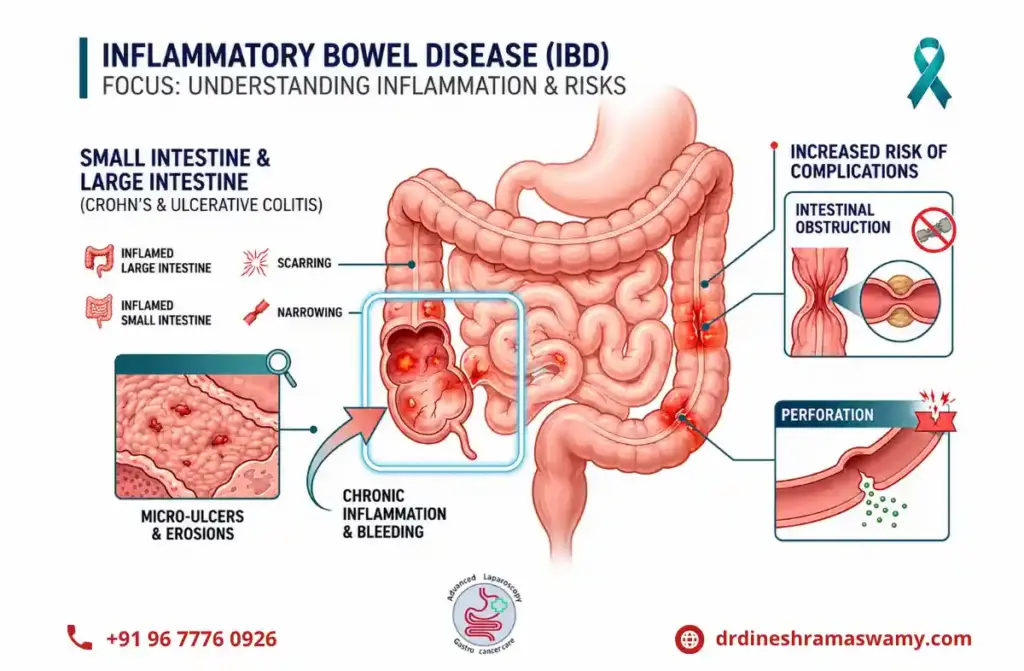
Crohn’s Disease is a type of Inflammatory Bowel Disease that can affect any part of the digestive tract, most commonly the small intestine and large intestine. It causes patchy inflammation that may spread deep into the intestinal wall, leading to pain and digestive complications. The symptoms may appear slowly over time and can range from mild discomfort to severe health issues.
Patients with Crohn’s Disease often experience:
- Cramping abdominal pain
- Chronic diarrhea
- Fatigue
- Weight loss
- Nutritional deficiencies
Some people also develop mouth ulcers, joint pain, and skin problems along with digestive symptoms.
Ulcerative Colitis
Ulcerative Colitis mainly affects the colon and rectum. Unlike Crohn’s Disease, the inflammation is continuous and usually limited to the inner lining of the intestine. Patients often experience urgent bowel movements and blood in the stool. Some individuals describe constantly searching for the nearest restroom due to frequent diarrhea. The severity may vary from mild inflammation to extensive disease affecting the entire colon.
Common symptoms include:
- Bloody diarrhea
- Abdominal discomfort
- Rectal bleeding
- Mucus in stool
- Sudden urgency to pass stool
Without treatment, repeated inflammation can damage the colon and increase the risk of complications.
The Silent Struggle of the Young
Inflammatory Bowel Disease (IBD) commonly affects people during their teens, 20s, and 30s — the most active and productive years of life. Persistent symptoms like abdominal pain, diarrhea, and fatigue can interfere with studies, careers, social life, and emotional well-being. Many young people continue to deal with the condition quietly because the symptoms are frequently overlooked or identified too late. Without proper treatment, IBD can significantly affect daily life and overall quality of life.
The Tuberculosis Trap
In many regions, particularly in India, the prevalence of Tuberculosis (TB) creates a unique diagnostic challenge. Since intestinal tuberculosis and Crohn’s Disease often present with similar symptoms and scan findings, they can sometimes be incorrectly diagnosed. Patients are often mistakenly put on anti-TB medication (ATT) while the actual inflammation from Crohn’s continues to damage the gut. Accurate diagnosis by a specialist at an early stage is important to prevent incorrect treatments and reduce the risk of serious long-term complications.
Common Symptoms of IBD
The symptoms of IBD can vary from person to person. Some individuals experience mild symptoms, while others face severe flare-ups.
Digestive Symptoms
- Abdominal Pain: Persistent stomach cramps or pain are among the most common symptoms. The discomfort often becomes more intense after eating or while passing stool.
- Diarrhea: Frequent loose stools lasting for weeks should never be ignored. Chronic diarrhea can lead to dehydration and weakness.
- Blood in Stool:Blood in stool may appear bright red or mixed with bowel movements. Many patients initially mistake it for piles.
- Bloating:Inflammation and digestive disturbances often cause abdominal bloating and discomfort.
General Symptoms
- Fatigue:Chronic inflammation drains the body’s energy, leading to constant tiredness.
- Weight Loss:Reduced appetite, poor nutrient absorption, and ongoing inflammation can cause unexplained weight loss.
- Fever:Low-grade fever may occur during active inflammation.
- Loss of Appetite:Patients often avoid eating because meals trigger pain or diarrhea.
Ignoring these symptoms for a long time can lead to complications such as malnutrition, severe dehydration, and intestinal damage. Many people mistake these warning signs for common digestive issues and delay medical consultation. Seeking early medical advice can help manage symptoms effectively and improve long-term digestive health.
How Is IBD Diagnosed?
Diagnosing Inflammatory Bowel Disease (IBD) involves a detailed evaluation of symptoms, medical history, and specialized diagnostic tests. Since IBD symptoms often resemble other digestive conditions, accurate diagnosis is important to identify the type and severity of inflammation. Early detection helps prevent complications and allows timely treatment for better long-term management.
- Physical Examination:Doctors check for abdominal tenderness, bloating, weight loss, dehydration, and signs of nutritional deficiencies. They also review the patient’s medical history and symptom patterns to understand the severity of the condition.
- Blood Tests: Blood tests help detect inflammation, anemia, infection, and vitamin deficiencies commonly associated with IBD. These tests also help doctors monitor the body’s immune response and overall health condition.
- Stool Tests: Stool analysis is performed to rule out bacterial or parasitic infections and identify inflammation in the intestines. It helps differentiate IBD from common digestive infections and other bowel disorders.
- Colonoscopy and Endoscopy: Colonoscopy is one of the most important procedures for diagnosing IBD, allowing doctors to examine the colon using a flexible camera. Tissue samples may also be collected for biopsy to confirm inflammation and identify the type of IBD. Endoscopy may be used to evaluate the upper digestive tract when needed.
- Imaging Scans: CT scans and MRI scans provide detailed images of the digestive tract and help detect complications such as intestinal narrowing, fistulas, or deep inflammation. These scans are especially useful in evaluating Crohn’s Disease.
Accurate diagnosis is essential because untreated IBD can lead to long-term intestinal damage and serious health complications. Many patients delay testing by assuming the symptoms are temporary digestive issues. Consulting a specialist early can help control inflammation, improve quality of life, and reduce the risk of severe complications.
Treatment Options for IBD
Although there is no permanent cure for Inflammatory Bowel Disease (IBD), several modern treatment options can help control inflammation, reduce symptoms, and improve quality of life. The treatment plan usually depends on the severity of the disease, affected area of the digestive tract, and the patient’s overall health. Early treatment and regular follow-up are important to prevent complications and manage flare-ups effectively.
Medications
Medications are commonly used to reduce inflammation and control the immune system response responsible for IBD symptoms. Doctors may prescribe anti-inflammatory drugs, immunosuppressants, or biologic therapies based on the severity of the condition. Many patients experience significant symptom relief with proper medical treatment.
- Anti-inflammatory Drugs: These medicines help reduce swelling and irritation in the digestive tract, improving symptoms such as abdominal pain and diarrhea.
- Immunosuppressants: Immunosuppressive medications control the overactive immune response that causes chronic inflammation in IBD patients.
- Biologics: Biologic therapies target specific inflammatory pathways and are often recommended for moderate to severe IBD cases when conventional medications are less effective.
Surgery options
- Ulcerative Colitis: In severe cases of Ulcerative Colitis, doctors may recommend a colectomy, which involves removing the affected colon. This procedure can help eliminate severe inflammation, bleeding, and recurring symptoms when medications are no longer effective. Many patients experience significant improvement in their quality of life after surgery. Regular follow-up care is still important for long-term health management.
- Crohn’s Disease: Surgery for Crohn’s Disease is usually performed to remove damaged or blocked sections of the digestive tract. It may help reduce severe pain, intestinal blockage, fistulas, or other complications caused by chronic inflammation. Although surgery can improve symptoms and digestion, Crohn’s Disease may return in other parts of the intestine over time. Ongoing medical treatment and monitoring are often required even after surgery.
Proper treatment and regular monitoring can help many patients live healthier and more comfortable lives with IBD. Ignoring symptoms or delaying treatment may increase the risk of complications and repeated flare-ups. Consulting a gastroenterologist early can help create an effective long-term management plan tailored to individual needs.
Complications of Untreated IBD
Ignoring IBD symptoms can lead to serious health complications.
- Malnutrition: Chronic inflammation in the digestive tract can affect the body’s ability to absorb essential nutrients properly. Over time, this may lead to vitamin deficiencies, weakness, fatigue, and unhealthy weight loss.
- Intestinal Blockage: Long-term inflammation can cause narrowing of the intestine, making it difficult for food and waste to pass normally. This may result in severe abdominal pain, bloating, vomiting, and digestive discomfort.
- Colon Cancer Risk: Persistent inflammation in the colon over several years can increase the risk of colorectal cancer, especially in patients with Ulcerative Colitis. Regular medical follow-up and colon screening are important for early detection.
- Severe Dehydration: Frequent diarrhea can lead to excessive loss of fluids and electrolytes from the body. Severe dehydration may cause dizziness, weakness, low energy levels, and serious health complications if untreated.
- Other Possible Complications: Some patients may also develop fistulas, abscesses, osteoporosis, liver disorders, and joint inflammation due to ongoing immune system activity. Early diagnosis and proper treatment can help reduce the risk of these complications.
When Should You See a Doctor?
Many people ignore IBD symptoms for months or even years, assuming they are caused by simple indigestion, food poisoning, stress, or unhealthy eating habits. However, persistent digestive problems should never be overlooked, especially when they continue for more than 2–4 weeks. Early medical attention can help prevent complications and improve long-term digestive health.
Consult a doctor if you experience:
- Persistent Diarrhea: Frequent loose stools that continue for several weeks
- Abdominal Pain: Recurring stomach cramps or pain, especially in the lower abdomen
- Blood in Stool: Rectal bleeding, mucus, or blood mixed with stool
- Unexplained Weight Loss: Sudden weight loss without changes in diet or exercise
- Chronic Fatigue: Constant tiredness even after adequate rest
- Fever with Digestive Symptoms: Low-grade fever along with diarrhea or abdominal discomfort
- Recurrent Bloating and Bowel Discomfort: Frequent bloating, gas, or irregular bowel habits
Ignoring these warning signs may lead to complications such as malnutrition, dehydration, intestinal damage, and increased inflammation. Consulting a gastroenterologist at the right time can help with early diagnosis, proper treatment, symptom control, and reducing the risk of severe flare-ups and long-term complications.
Preventive Measures for IBS
Although IBD and IBS are different conditions, certain digestive health habits may help reduce irritation and improve gut function.
Key Prevention Strategies
- Identify Dietary Triggers: Keeping a food diary helps identify foods that worsen symptoms. Common triggers may include dairy, caffeine, fried foods, and spicy meals.
- Follow a Low-FODMAP Diet: A Low-FODMAP diet reduces certain carbohydrates that may trigger bloating and digestive discomfort in sensitive individuals.
- Increase Soluble Fiber: Foods rich in soluble fiber, such as oats, bananas, and apples, may support digestive balance.
- Eat Smaller, Regular Meals: Large meals may overload digestion. Smaller meals eaten regularly are often easier to tolerate.
- Limit Processed Foods: Reducing processed snacks, sugary foods, and artificial additives may improve gut health.
Lifestyle and Mindset Changes
- Manage Stress: Stress management is important because emotional stress can worsen digestive symptoms.Meditation, walking, journaling, and relaxation techniques may help maintain emotional balance.
- Regular Exercise: Physical activity supports digestion, circulation, and overall well-being.Even simple activities like walking or cycling can make a difference.
- Ensure Adequate Sleep: Poor sleep may worsen inflammation and fatigue. Consistent sleep habits support immune health.
- Stay Hydrated: Frequent diarrhea can lead to dehydration. Drinking enough water is essential for digestive function and recovery.
Conclusion
Inflammatory Bowel Disease (IBD) is a chronic digestive condition that can affect physical health, emotional well-being, work, and daily life. Symptoms such as abdominal pain, diarrhea, blood in stool, fatigue, and unexplained weight loss should not be ignored or mistaken for common stomach problems. With early diagnosis, proper treatment, healthy lifestyle changes, and regular medical care, many patients can successfully manage symptoms and maintain a better quality of life.

